(Author’s note: I wrote this over a sixteen-month period. It is too long and needs a stern editor. It isn’t dramatic or particularly compelling. It’s just a story about have cancer.)
I have cancer. I’ll repeat that. I have cancer. The tumor is dying, but it’s still considered active. Regardless, it’s not a cancer “scare,” although it is quite scary. It’s the real thing—a malignant tumor in my prostate gland. Medically, it’s an adenocarcinoma. Cancer.
I was 56 when I was diagnosed, not particularly young or old for prostate cancer. I found out in July of 2019. I got a phone call, and the doctor said something to the effect of “We have your biopsy results. You do have malignant cells in your prostate. It’s a low to intermediate grade tumor. It’s very slow growing, but at your age you probably want treatment. We’ll call you back today for an appointment to talk about it. Any questions?” Despite having rolled around numerous nightmarish scenarios for four weeks, I really didn’t have any questions. My only thought at the moment was “Huh. Well, that’s weird.”
About a month before my biopsy, I had my annual physical. By “annual,” I mean the physical examination I have every few years. My last one was four years ago. In all humility, I must say that I am in tip-top physical condition–so, why go to the doctor, right? Apparently, most men my age are big messes. Okay, so my cholesterol should be a tad lower. Oh, and my PSA level was elevated—two and half times higher than before.

PSA. Prostate Specific Antigen. Long story short, it’s something produced by your prostate gland for various reasons. One reason is cancer. Mine went up a pretty fair amount in four years. I also had my prostate examined. It’s examined by something called a “digital rectal examination.” “Digital” doesn’t have anything to do with any sort of high tech diagnostics. It’s “digital” as in “finger,” just in case you aren’t aware of how it works. So, after my PSA test and DRE, my doctor thought I should see a urologist for more blood work and, of course, more DREing.
So, I saw a urologist. Great guy. I’m pleased to report that my prostate gland is remarkably small for a man my age. In fact, my urologist says that it’s the “prostate of a 20-year-old.” I guess he means a 20-year-old with cancer, but still…. My incredibly small prostate was something of an indicator of cancer, believe it or not. The increased PSA could have been caused by an enlarged or infected prostate. Mine was in pristine condition.
I’ll admit something. I didn’t know much about the prostate gland until all this. Given my age, I knew well the hideous DRE, but I really didn’t even know precisely where the prostate is located. Now, I know WAY more than I ever thought I would. Naturally, I have thoroughly searched the internet for every hideous prostate cancer story I can find. Did you know that Frank Zappa died at 51 of prostate cancer? Bill Bixby was 59. Gary Cooper was 60. Basketball player John “Hot Rod” Williams was 53. Then again, a lot of really old guys die of prostate cancer, too. Dennis Hopper, for instance. He survived the ‘60’s and countless drug-fueled adventures. He didn’t survive this, though. There’s even a Wikipedia listing people who died from prostate cancer. I’ve studied it. Intently.
Men, if you live long enough, you’ll have prostate problems. You’ll probably have prostate cancer at some point. Like all cancer, the keys are: 1. When you get it; 2. When you find out you got it; and 3. How aggressive it is. Unlike some cancers, it can be treated. Like all cancers, if you wait too long to find out about it, it can also certainly kill you.
Well, my cancer wasn’t going to kill me, at least not any time soon. I was repeatedly assured of that. My oncologist even said, “You’re not going to die from this.” I really appreciated being told that, even though I was able to convince myself that I still might be dying.
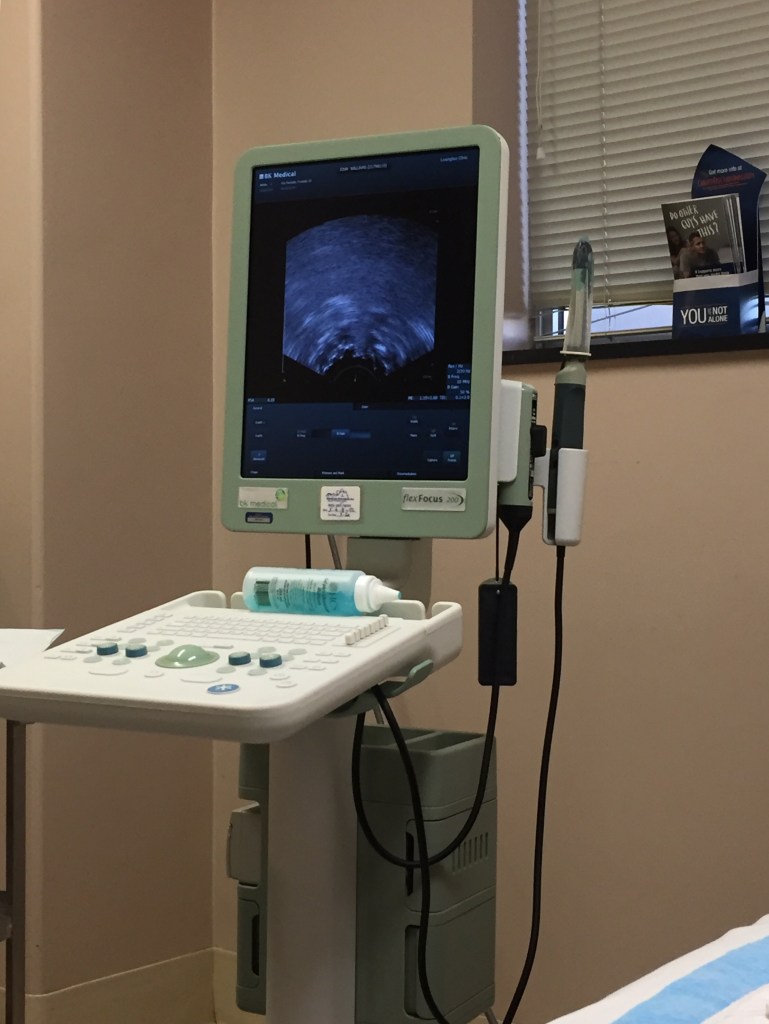
In addition to the blood tests and DREs, I also had a biopsy. It was unpleasant. As with all prostate-related procedures, it involved rectal probing. Basically, a metal rod is inserted, then your prostate is located by ultrasound through the wall of your large bowel. After that, a needle is shot into your prostate numerous times to take tissue samples. All in all, it’s pretty painless, as rectal probing goes. Oh, there’s some revolting bleeding that goes on for a few days, but it’s not that big a deal.
All this happens, and then they tell me it’s cancer. It gets a Gleason Score which is a complicated scoring system using charts that get cross-referenced to give your grade. It’s all rather mechanical. More good news. My score wasn’t too high. Low to intermediate grade adenocarcinoma. That means it’s all inside the prostate—most likely. Now, you have to figure what to do.
This all sounds pretty positive, doesn’t it? Well, it is given the context, yet it was still terrifying. Even though there were some pretty strong indications before the biopsy that I had cancer, I still didn’t really think I had it. It just didn’t seem like something I would have. I’ve never been hospitalized for anything. I’ve never had surgery. Or a CT scan. Or an MRI. The only broken bones I’ve had were two small stress fractures on the top of my right foot about 20 years ago.
After the news sank in, I began to consider that this is the end for me. I’ll find out it’s some sort of unmanageable cancer that runs wild. I was reminded of my wife’s grandmother who liked to regale us with dire stories of her friends who were deathly ill. Once asked her what type of cancer one of her unfortunate friends had. Granny said: “The fast-eatin’ kind.” I figured I had that, too. Like most things that terrify me, it actually never happened. Mine was the “slow-eatin’ kind.” Regardless, there’s still a ton of stress. It’s just weird to think I have cancer. For example, when the dentist asked if I’d had any changes in my health, I had to say “Oh, yeah, I have cancer.”
In the majority of cases—mine included—prostate cancer is slow-growing. I could go a number of years doing nothing before I have major problems. That’s actually one option. Do nothing. Monitor the situation and then act when necessary. That approach wasn’t recommended for me, because I’m relatively young in the prostate cancer world. Plus, I wouldn’t deal well with the stress of being checked every six months or year. So, I had to pick a treatment option.
My choices were radiation, surgery or something called HIFU (High Intensity Focused Ultrasound). HIFU wasn’t covered by insurance, so it was a nonstarter. There are three kinds of radiation treatment: 1) External beam; 2) seed implantation; and 3) CyberKnife. Surgery is just what it sounds like. They cut out your prostate gland. My decision came down between CyberKnife and surgery. I’m not a good candidate for the other radiation treatments for a number of reasons. That’s good, because they’re really intense.
Surgery is the most conservative approach. You cut it out and have thorough pathology done on the gland and know exactly what you’re dealing with. As you might expect, though, there are some real negatives, too. How about walking around with a catheter for at least a couple of weeks? Bladder leakage for some period time or forever. Possible impotence. These are worse case scenarios, of course, but the doctors are blunt about the possibilities. If it came down to courting death or dealing with all this, I wouldn’t have hesitated on the surgery. Fortunately, that wasn’t the case with me. Side effects aside, I’m not real keen on being cut on unless it’s necessary.
I chose CyberKnife. CyberKnife is a high-intensity radiation beam that targets the prostate and then “slices” the tumor up. The goal is to kill it. If it doesn’t not kill it, you want to at least slow it down enough that something gets else you first. Why do this? Turns out I’m a great candidate. I’m very fit. I’m not overweight. My tumor is small and low to intermediate grade. Everyone was quite confident about the treatment.
Of course, this isn’t without its own side effects. There’s fatigue for a two or three weeks. or so. There are the dreaded “frequent loose stools.” The GI issues were minor–more annoying than anything else. All things considered, it’s not so bad.

So, I had the treatment. I laid on a table and a huge piece of equipment moved around me for about 45 minutes. I had to lie perfectly still. I listened to music. They put a warm blanket over me. Not bad, right? Well, it was a tad scary. In fact, I almost hyperventilated before the first treatment. While I was lying there, it suddenly struck me that I must have something seriously wrong with me. Otherwise, they wouldn’t be doing this to me. Plus, everyone was REALLY nice to me. This is how all patients should be treated.
I forgot about the enemas. I had to have one every morning before my treatment. I had to do it myself, which is preferable I suppose. After a while, one more thing up in there is no big deal. I also had to go on weird “low residue” diet which was about as bland as it sounds.
The treatments were weird. I didn’t feel anything. It didn’t seem like anything was happening, but I knew it was. I knew because no one could be in the room with me while it was happening.
There were side effects. Fatigue was the major one. A couple of days after the last treatment, I started hitting a wall in the afternoon. I’m an active guy. Crazy active. I work out every day, and I did so after my treatment, but I had to work around the fatigue. When it hit, it was like catching the flu in about five minutes. My legs would die. I’d be sleepy, almost achy. It passed after an hour or two, quicker if I could grab a nap.
It took a couple of weeks to start feeling better, but I did. By Christmas, I was hale and hardy again.
There were some urinating issues. The less said about that the better, but it wasn’t so bad. I took one one pill a day for that, and it helped.
So, here’s how we got here:
June 11, 2019: I have my periodic physical. Doctor calls later in the day to talk about my PSA level. It’s not good when your doctor personally calls you on the same day you have a physical.
July 8, 2019: Biopsy.
July 16, 2019: Biopsy results.
August 21, 2019: Meet with urologist to discuss options.
September 12, 2019: Meet with surgeon to discuss surgical option.
September 26, 2019: Meet with radio-oncologist to discuss radiation treatment. That same day, I decided to go with CyberKnife.
October 28, 2019: Fiducial markers inserted into my prostate. These are four pieces of gold about the size of grains of rice. They put in through a needle—again, more rectal probing. These markers make the prostate–and tumor– easy to locate. Unpleasant, but as cancer treatment goes, not that bad.
November 11, 2019: X-rays, CT scan and MRI to prepare a treatment plan. My markers are located and something of a map is created for the CyberKnife to follow in zapping my prostate.
November 25-27 and December 2-3: Treatment.

Not much happened after that. I saw my urologist on March 11, 2020. Good news. My PSA level was cut by a third. The doctor and I also talked about this new virus “COVID-19.” He said it looked like really serious stuff and that I should be sure to frequently wash my hands. It sounded like we might be in for a rough few weeks.
Another physical in June 2020 (those will be ANNUAL from now on.) More good news: PSA level cut in half. Then, a follow up visit to the oncologist. He says I’m right where I should be. He’s confident the tumor is dying. I have one more appointment in July 2021, and he expects to release me from treatment. Whew.
In September 2020, I went back to the urologist. By the way, you can’t have a prostate exam during a telehealth appointment, so it had to be face-to-face, or something like that. PSA has fallen even further. Doctor says I’m clearly on my way to full recovery. He took me off my prostate medication.
So, that’s cancer my story (so far). As comic Norm MacDonald says, the best news you get from a doctor is that nothing is wrong with you…YET. Mine isn’t a dramatic tale of survival. I wrote this so I could remember it. The fog of time obscures a lot details. Plus, I want to share it with others who might be in the same situation.
Fifteen doctor/clinic visits; seven prostate exams; seven enemas; one biopsy; one procedure to implant the fiducial markers; and five radiation treatments: Not so bad as cancer treatment goes. Yet, I’m pretty that’s more medical treatment than I’ve had in test of my adult life.
I also learned a lot. In the past, I would hear of people with “non-serious” cancer and think “Well, that’s unfortunate, but it sounds curable. Good for him.” I don’t think that way now. It’s a chilling to be told you have cancer. It’s scary. It’s confirmation of your expiration date—if not now, it’s coming.
I also appreciate doctors and science in a new way. I’ve lived my whole life in Kentucky, and I love it here. Unfortunately, during the COVID pandemic, I learned that many Kentuckians don’t care much for science. They also come up with their own science. If you want to become a fan of science, get cancer. You’ll be all about science then. You won’t be looking for memes or your politicians to tell you what to do. Doctors will do quite nicely.
I can’t overstate how well I was treated. All my questions were answered. If I called, someone PROMPTLY called back. Everyone was nice. The way I am, it made me think I might be really sick. Why else would they be so nice?
I was likewise impressed by the effort to fully educate me. I got recommendations along the way, but the choices were mine.
Big thanks to my primary care doctor Dr. Eiyad Alchureiqi at Lexington Clinic; Urologist Dr. Stephen Monnig at Lexington Clinic; Dr. Alan Beckman, my radio-oncologist at Baptist Healthcare. They and their staffs were top notch from start to finish. My wife, too, deserves HUGE thanks. She was optimistic from start to finish. I needed that.
Here are few lessons I learned:
- DON’T tell a cancer patient about that person you know who died of the VERY SAME THING. No one wants to hear that. Your medical opinion is also not likely to be well-received. Okay, so you know a guy who had the same treatment, and it failed miserably. Keep it to yourself.
- DON’T tell a cancer patient that he or she should have opted for some other form of treatment. He or she is making a decision based on the available information. Don’t invite second-guessing.
- DON’T pry. Here’s the best thing to say: “How are you?” If the person feels like telling you–believe me–you’ll find out. If I feel like telling you that I’m have trouble peeing, I’ll let you know.
- DON’T pander. “I’m sure you’ll fine” and the like really don’t mean anything. Unless you’ve had experience with a similar situation, you don’t know if someone will be “fine” or not.
- DO be empathetic. I tend to dwell on myself which results in nothing good. This flaw was especially acute after my diagnosis. No matter how bad something seems, someone else has it worse. Just sit in the waiting area at a cancer center, and you’ll see. Think about others. Consider what you would do if you couldn’t get treatment or it didn’t work.
I’ll never look at people with cancer the same way. Cancer is like surgery. “Minor” cancer is someone else’s cancer. I’ve even heard people saying that cancer can be a blessing. I don’t agree, especially for the many folks I’ve known who have been seriously ill or have had debilitating forms of treatment. So, if you have or had cancer, I have, too.
©thetrivialtroll.com 2020